Typical day in Recovery
Click on the heading below to find out what they might be doing at that specific point in the day.
As with any role within the NHS confidentiality, data protection and security is paramount before entering any clinical environment.  Usually entry will require authentication via security access passport, security codes or even buzzing to gain entry onto the premises. A professional attitude is vital and staff (including students) have a certain obligations to uphold when entering the clinical setting.
Usually entry will require authentication via security access passport, security codes or even buzzing to gain entry onto the premises. A professional attitude is vital and staff (including students) have a certain obligations to uphold when entering the clinical setting.
Shift patterns may vary where some may start work earlier than others dependant on duties for that day. usually Anaesthetics may start first with Recovery starting later and probably finishing later dependant on the patients needs.
As a student you will be required to work Monday to Friday and you may be expected to work 'out of hours' to experience emergency and trauma care.
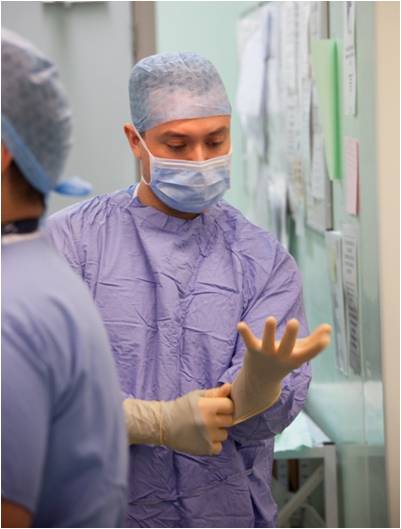 On entering the department staff will proceed to the changing rooms in preparation for entering a clean environment. 'Dress codes' and cleanliness are major protectors against hospital infections, and proper preparation to enter a surgical environment is vital. This will mean the removal of all jewellery, with few exemptions and the donning of theatre scrubs as per local hospital policy.
On entering the department staff will proceed to the changing rooms in preparation for entering a clean environment. 'Dress codes' and cleanliness are major protectors against hospital infections, and proper preparation to enter a surgical environment is vital. This will mean the removal of all jewellery, with few exemptions and the donning of theatre scrubs as per local hospital policy.
Dependant on speciality this may vary from Scrubs and shoes, to in some case full scrubs, shoes, hat and mask. Scrubs are supplied by the Trust whilst specialist theatre shoes are worn to minimise cross contamination from the outside world.
Many operating departments work on the policy the closer to the patient operating room the cleaner the environment.
One of the biggest impacting factors on daily workload is the constant changing of duties on a day to day basis. Many times you will leave the previous day thinking you are in one theatre and the next morning due to emergencies for example everything may have changed, not only might you be in another theatre, but it might even be an entirely different speciality. Generally you will be where planned but with increasing experience comes increasing responsibility to the service.
To meet these challenges communication punctuality, organisation and team working are essential qualities in a potential ODP.

These are suggested total and do not represent any individual organisation, as many will have their own policies and procedures to maintain.
Click to learn more about the role of the nurse
The recovery practitioner, after collecting the operating list containing all the session procedures, order of play and specialist requirements will start to prepare the recovery area. These checks might include
- Checking recovery bays,
- Preparing work surfaces
- Ensuring all specialist equipment is in situ
- Making sure all the drugs required for the list are available and are at hand
- Ensuring that emergency equipment is available if required
- Checking that the operating table is correct and set up appropriately for the first case.
Communication amongst the Multi Disciplinary Team (MDT) is paramount at this stage. It is vital that the team communicate with each other to confirm that all the necessary equipment is available when required, all the staff are ready to commence the operating list.
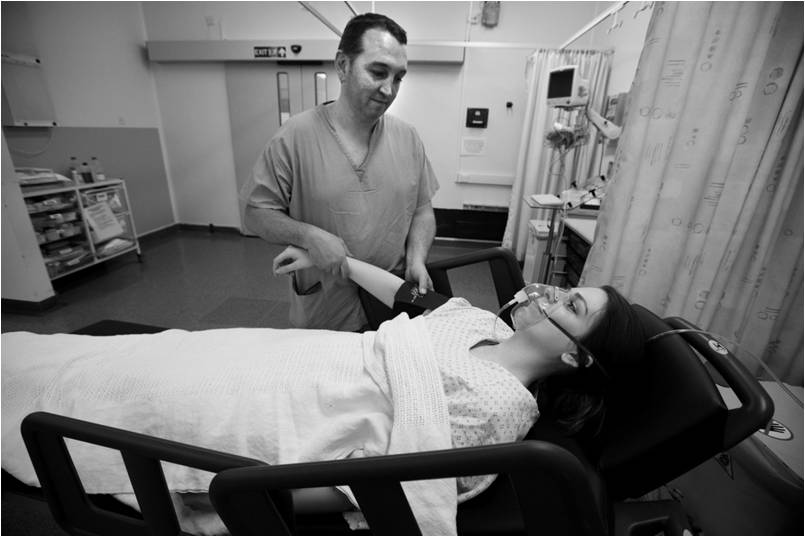 Recovery from the surgical procedure and the anaesthetic begins on the operating table. Once all the counts have been completed satisfactorily, the patient cleaned and all the appropriate aftercare dressings applied the patient is slowly reversed from the anaesthetic. The main function of the team here is to prepare the patient for transfer to the recovery area.
Recovery from the surgical procedure and the anaesthetic begins on the operating table. Once all the counts have been completed satisfactorily, the patient cleaned and all the appropriate aftercare dressings applied the patient is slowly reversed from the anaesthetic. The main function of the team here is to prepare the patient for transfer to the recovery area.
The Anaesthetic ODP will assist the Anaesthetist in making sure the patient is both comfortable and pain free. In some organisation this role may be carried out by a recovery ODP. The surgical team will also assist in the safe hand over of patient specific information to the next treatment area.
Once the patient is able to be transfer and leaves the theatre, preparation for the next procedure begins.
This is everyone's role with in the team. All clinical waste from the previous procedure needs to be removed safely following  organisational protocols for hazardous waste. All surfaces must be cleaned and prepared for the next case.
organisational protocols for hazardous waste. All surfaces must be cleaned and prepared for the next case.
In the case of anaesthetics this will include preparation of the anaesthetic machine which may require a complete recheck to ensure all is in working order.
The operating table may need altering for different procedures, in the case of Orthopaedics this may mean a completely new table as some procedures will need the traction attachments assembling.
New specialist equipment might be required. In the case of a general list the first case may have been an open procedure whilst the next could be laparoscopic .
In recovery this will mean cleaning and restocking of the different bays that the patients utilise.
The patient is cared for until they are able to, with assistance if necessary, take care of their basic functions e.g. breathing. Pain relief is monitored and administered following surgery and only once the patient is safe to transfer are they taken to their bed on the ward.
The day can be tedious, hard working and sometimes downright boring, certainly there are the exciting times when people are desperately trying hard to save a life but they are few and far between. Standing for long periods whilst scrubbed or watching monitors during long cases observing no change in patient's vital signs are normal everyday occurrences in the life of an ODP. The role has it's rewards but sometimes staff can feel that much of their work is unchanging and sometimes feel that little recognition is awarded for all their efforts.
During winter periods it is normal to go to work in the dark and come home in the dark and sometimes not see daylight for a week simply as most operating departments are unusually placed in the basement and have no external windows.
The role is life changing in many ways so due consideration is required, the rewards as stated earlier are plentiful, but the cost can be at times be extreme.
